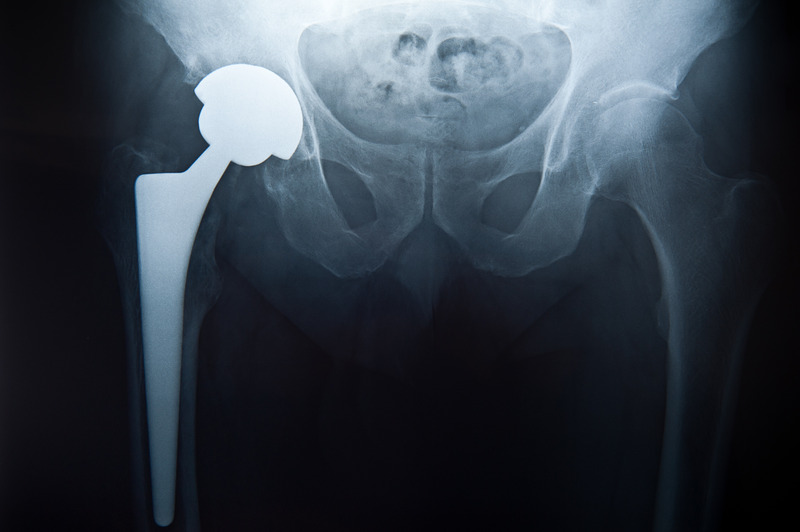
In order to help you recover after hip surgery, we’ve created this help Hip Replacement Guide
Are metal ions only present for one year after surgery?
No. It is well documented that metal ion levels are higher in the first one to two years after implantation of metal-metal bearings. After this initial “run-in” period, the levels drop to a much lower constant rate for the remainder of the implant life.
What is an FDA-approved implant?
When a medicine or implant is approved for sale by the FDA, it is approved for a set of specific indications (uses). The manufacturer is limited in marketing the medicine or the device for only certain indications that have been reviewed and approved by the FDA. However, physicians and surgeons may use these medicines and implants for other reasons (off-label use) only medical doctors have the necessary knowledge, training, and professional judgment to decide when and where medicines and implants are to be used appropriately.
Our right to exercise this judgment is bestowed on us by our medical license. Insurance companies, hospitals, and other healthcare entities do not have a license to practice medicine. The FDA realizes that it is impossible to require separate testing and approval for each possible individual use of a medicine or implant, therefore the government has developed this two-tiered approach to regulation.
What is an FDA procedure?
This exists only in the minds of insurance companies. The FDA only approves devices and medicines.
Why do total hip replacements dislocate?
Because a hip replacement typically has a smaller bearing than your natural hip joint. The natural hip joint only rarely dislocates with extreme trauma (a fall from a second story, or a severe motor vehicle accident where the knee is driven against the dashboard). However, a traditional total hip replacement carries a 5-7% lifetime risk of dislocation, without significant trauma. This is because a total hip replacement relies on a mechanically unstable small bearing.
To provide a plastic bearing surface and a socket that is thick enough to last, the femoral bearing size needs to be reduced to a much smaller size (average size 28 mm), than the natural hip (size 44-56 mm). Similar small bearing sizes are also required for ceramic on ceramic implants. This leads to a 5-7% risk of dislocation over the lifetime of the implant. However, very durable modern metal-on-metal bearings can be manufactured with very thin (3-6 mm) acetabular components. This allows the use of a large femoral component (either THR or HSR) that allows for retaining the natural stability of the hip joint. Large-bearing metal on metal TKR and HSR rarely if ever dislocates.
Why are there so many restrictions with Total Hip Replacement (THR)?
There are two reasons. First, most traditional hip replacements are inherently unstable. Permanent hip position precautions are required to avoid dislocations. Secondly, bearing surfaces can wear out or fracture. Studies in young active patients indicate a 20-30% failure rate by 8 years with standard polyethylene bearings. Crosslinked polyethylene and ceramic on ceramic bearings are more durable to wear. However, they are still prone to crack with severe repetitive impact activities. Only large metal-metal bearings are stable and durable enough to allow full activities without restrictions.
Can you lengthen my leg with a hip replacement?
With HSR typical leg lengthening is _ cm (3/16 inch). In certain cases of hip dysplasia or severe acetabular wear up to 1 cm (3/8 inch) increased length can be achieved. In THR the leg can be lengthened up to 2.5 cm (1 inch). In THR occasionally it occurs. This cannot occur with HSR.
What is the advantage of minimally invasive surgery?
The advantage is less postoperative pain and a better cosmetic result as well as a more rapid healing time. We can now discharge most patients from the hospital within one to two days after surgery using these techniques.
What is the best bearing surface in hip replacement?
Metal on a metal bearing is the best choice for hip replacement for the following two reasons:
- Metal is an extremely durable surface that is unlikely to ever wear out.
- Stability of the joint. Using metal on the metal bearing surfaces allows the manufacture of a large bearing hip joint that will not dislocate. Traditional hip replacements are not durable enough for many of today’s younger more active patients. Traditional metal on plastic bearing devices has been shown to have a failure rate of (30 % ) by seven years in this patient group. Recently several new bearing couples have been developed as more durable options:
- Crosslinked polyethylene – more durable than standard plastic but still not well tested. Previous modifications in plastics have been very unsuccessful.
- Ceramic on Ceramic – very durable bearing surface. Unlikely to ever wear out. However, the manufacture of this brittle material is very tricky, occasionally failing by fractures of the ceramic parts while in use.
- Metal-on-Metal – very durable bearing surface. Unlikely to ever wear out. No possibility of cracking like ceramic. Although metal-on-metal and ceramics are equally durable bearing surfaces, the metal-on-metal bearing has one distinct advantage over all other bearing surfaces.
Large-diameter joint replacements can be manufactured which allow the surgeons to reconstruct the hip in a mechanically sound fashion similar to a patient’s original hip and thus avoid dislocation after surgery. This is a major advantage that should not be underestimated. It is estimated that 5-7% of patients with total hip replacement will suffer dislocation over ten years; with large bearing joints the chance is less than 1%.
The improved stability makes it possible for us to offer patients a new hip without all of the traditional restrictions of total hip replacement restrictions used to include no deep bending, crouching, or crossing legs). Patients can now kayak and participate in dance, gymnastics, martial arts, etc. There is one potential problem with metal-on-metal bearings. Normal wear results in the release of metal particles into the body.
One problem with any artificial bearing surface is the wear regenerated by normal daily wear and tear. Large volumes of plastic generated by metal-on-plastic (traditional) replacements result in large amounts of bone destruction, (osteolysis) around implants and have been the major cause of failure in young patients. Both ceramic-on-ceramic and metal-on-metal devices generate about 99% less wear debris than traditional bearings and the debris generated seems to cause less irritation to the bone than plastic debris does. There has been some speculation about the potential for metal debris to cause cancer. However, with careful studies to date, no links have been demonstrated. The advantage of metal-on-metal bearings strongly outweighs the potential risks.
Now we can return patients to normal function with almost no restrictions and expect their implants to last more than 10 years at very high activity levels. Most patients will never require another operation on their hip. If ceramic-on-ceramic or metal-on-crosslinked polyethylene bearings are used, wear is also not a problem, but significant restrictions remain. No running or jumping can be allowed due to the risk of fracture of the implant: no crossing of the legs or extreme bending can be allowed due to the risk of dislocation.
What complications can occur?
We perform a high volume of knee and hip joint replacements (currently over 400 per year). Detailed risk disclosures based on our results for primary straightforward surgery are available on Forms #10, #11, and #12. Please note that most general medical complications are not specified in detail because they vary according to the general health and age of the patient. Also complex or revision cases have significantly higher rates of complication.
Why are most surgeons not performing hip surface replacement?
Originally it was thought that hip surface replacement did not work because of the high rate of avascular necrosis (AVN) of the femoral head and a high rate of femoral neck fractures (over 30% in three years). However, we now know that this is not true. In the 70’s and 80’s, hip surface replacement was done with metal-on plastic bearings. It is now clear that the failures in the past were primarily due to rapid wear of the plastic bearings resulting in extensive bone destruction (osteolysis). With modern cobalt chrome metal-metal bearings, the rate of femoral neck fractures has dropped to 1% and the rate of AVN to 2%. Most surgeons are not aware of this. The second reason is that the operation is much more difficult to master compared to total hip replacement. Many surgeons are simply not willing to learn these techniques and some just don’t have the surgical skills to attempt to learn this technique. Only those surgeons who already perform a high volume of hip surgery, and are willing to dedicate a lot of time and energy to master this procedure, should attempt hip surface replacement.
What surgeons perform hip surface replacement?
There are only 10-20 surgeons in the US who have significant experience with this procedure at this time (March 2007). We currently have the second largest individual experience in the US with over 1100 cases performed.
Is hip surface replacement experimental surgery?
NO. It has been performed since the advent of joint replacement in the 1950s. Past implant systems were not durable enough; therefore stemmed total hip replacement has become the standard operation for treating severe hip arthritis. With modern cobalt chrome metal-metal bearings, there has been a worldwide resurgence of this operation. The US is far behind the rest of the world, primarily because the FDA has made obtaining modern implants extremely difficult.
In England, approximately 12% of hip replacements are now done as hip surface replacements. In Australia, 20% of hip replacements are done as hip surface replacements. The percentages continue to grow; Europe, Australia, and even India are ahead of the US! There are now many published articles in peer-reviewed journals and presentations at major orthopedic meetings on this subject. At this point, some insurance companies still find it convenient to classify hip surface replacement as experimental in order to avoid paying for this service. Despite the fact that it is truly in their best interest to cover this procedure; the costs and complications are less than Stemmed THR.
How long is the recovery?
Using minimally invasive techniques, advanced multimodal pain management, and rapid progression of physical therapy, the recovery is quite rapid. The hospital stay for total hip replacement or hip surface replacement is only one or two days and most patients do not even finish taking their prescription narcotic tablets after they go home. Crutches are only used for one to two weeks and return to work is quite rapid. By six weeks postoperatively most patients have significantly less pain than before surgery and walk one or two miles with a slight limp. Full healing occurs by one year.
What is the advantage of a hip surface replacement?
There are pros and cons. The advantages include:
- Less bone is removed.
- It is more durable than standard total hip replacement in young people (96% survivorship at 8 years in the English literature).
- Stability is better: a. no dislocation b. Minimal early postoperative hip precautions c. No hip precautions after 6 months.
- No thigh pain.
- Less risk of blood clots (3 in 700, compared to 10% with total hip replacement).
- Less blood loss in surgery (transfusion is required in less than 1% in patients with a preoperative hemoglobin greater than 13; there is no need for autologous blood collection).
Recently large bearing metal-metal total hip replacements have become available as well (Biomet Magnum, released 12/2004 in the US market). We expect them to be just as durable and stable as hip surface replacement. The disadvantages of hip surface replacement include: % 1. 1% femoral neck fracture.% 2. 2% femoral head avascular necrosis. Both of these complications require revision of the femoral side to a large bearing implant that will mate with the acetabular component in place.
Do metal ions pose a health risk?
Implants containing a metal-metal bearing result in higher metal ion levels in your body. To a lesser extent this is true of any metal implant including all total joint replacements, even those with ceramic or plastic bearings. There is speculation put forth primarily by proponents of bearing surfaces other than metal-on-metal that elevated levels of metal ions are harmful.
There is no credible evidence that this is actually the case. Cobalt and chromium ions are native to your body and are commonly taken as supplements in most multivitamin preparations. Some people also take additional mineral supplements with the belief that there is an added effect. Polyethylene and ceramic are completely foreign to our body. Multiple studies have shown that they are found throughout the body in the lymph system as well as in the liver. One could certainly speculate about the harmful effects of these materials.
The truth is that there is no credible evidence that any of these foreign particles cause long term problems in our bodies. Of course, we would prefer to have no foreign particles present if we had a choice. The best long-term study available on metal-metal bearings and possible cancer risks is by Dr. Visuri published in the journal Clinical Orthopedics and Related Research in 1994. It indicates no increased cancer risk with metal-metal implants in 450 patients over 15 years.