More studies may need to be done outside of the hospital to help us choose the best way to treat hip arthritis in the patient. For the studies noted below, our office will gladly assist you with scheduling.
Magnetic Resonance Imaging (MRI) Can Help Treat Hip Arthritis
Magnetic Resonance Imaging (MRI) is a very useful study, but it is often overused as well. It is well known that there are many false positives and false negatives. Often, physicians who are not orthopedic surgeons order expensive ($1500) scans when a simple x-ray would tell an orthopedic surgeon what the problem is. Most general physicians are not used to interpreting x-rays on their own. In this instance, the MRI has just wasted money. Orthopedic surgeons should only order musculoskeletal MRIs after they have evaluated the patient (costing $300). This would result in large savings in health care.
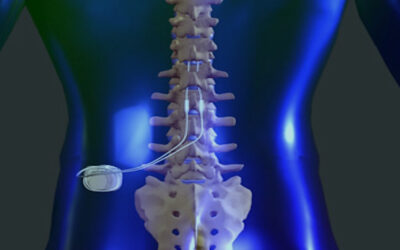
Many people believe that you cannot have an MRI if you have implanted metal. This is not true. Most implanted metals are not ferromagnetic and are not affected by the MRI magnets. The exceptions are metal fragments that get into the body accidentally, including shrapnel as well as cardiac pacemakers. MRI-compatible pacemakers should be available soon.
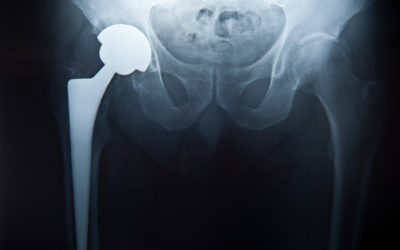
If an MRI is taken around an orthopedic implant, there is no danger to the patient. The metals we use—stainless steel, cobalt chrome, and titanium—are not magnetic. The problem with scanning around an implant is that an artifact is created around the implant on the diagnostic image. This artifact makes the image difficult to interpret. New software to eliminate this artifact has been developed and is called metal suppression or metal artifact reduction sequences (MARS). Not all radiologists know about these, and sometimes useless scans are still done around implants. The radiologists we use are well-versed in these techniques, but sometimes patients who don’t live here need to get scans done near their homes. You should find a larger center with a subspecialist in musculoskeletal radiology who can do the scan right.
In most cases of moderate to severe arthritis, an x-ray is all that is needed to make the diagnosis. Hip dysplasia, various impingement deformities, and stages 3 and 4 necrosis are also best evaluated by simple x-rays. A hip MRI is a useful study to look for problems such as stage 1 and 2 osteonecrosis, hip abductor tears, and labral tears. An arthrogram MRI (dye is injected into the joint before the MRI) is better when we look for a labral tear.
MARS MRI and Metal Suppression CT
If metal ion testing shows that there are too many metal ions, MARS MRI and metal suppression CT can be used to find out what is wrong with metal adverse wear failures (AWF).
Before hip replacement surgery, an MRI is needed to create 3D virtual models of the operative leg and plan the surgery. The company that provides this service creates sterile custom guides according to our protocol that is used in surgery to improve the accuracy of the bone, resulting in more reproducible alignment of the implants.
Finally, MRI is very useful to evaluate the lumbar spine for arthritis, herniated discs, and stenosis. These conditions may cause referred hip pain, confusing both the patient and the orthopedic surgeon. This is particularly useful after hip replacement if there is residual buttock, lateral hip, or sciatic pain.
CT Scans for Hip Arthritis
In some situations, CT scans can also be used to look for signs of adverse wear failure (AWF) around metal bearings. Similar to simple x-rays, but unlike MRI, they do expose the patient to a low dose of x-rays. They are less costly and allow imaging of both hips simultaneously. Metal suppression techniques also need to be used.
We are currently working on advanced techniques to accurately measure implant positions in 3 dimensions on these scans. This will help us make more accurate guidelines and surgical guides that can be put in place during surgery.
DEXA Scans for Hip Arthritis
DEXA scans (dual-energy X-ray absorptiometry) are the test we use to measure bone density. The result is reported as a T-score, which is a way to compare a patient’s bone density to that of a normal young population. Because bone density varies according to race and gender, different normal populations are used. A T score between 1 and -1 indicates that your bone density is within the range of 90% of the 26-year-old normal population of your reported race and gender.
If your T-score is below -1.5, you are said to have osteopenia. If it is below -2.5, you have osteoporosis. This means weak bones. These cutoff levels are arbitrary. The lower your bone density, the higher your fracture risk. Osteoporosis, unlike osteoarthritis, is not painful. Pain occurs when a bone breaks. Bone density gradually decreases with age for the entire population. Women can have a more rapid rate of decline in their bone density for the first 5 years after the onset of menopause. All women should have a baseline DEXA scan when they start menopause, and this should be repeated at least once 2 years later.
Neither condition is typically symptomatic. These conditions, if left untreated, will eventually lead to serious medical problems, such as heart attacks and strokes on the one hand, and fractures on the other. Both conditions can be treated to prevent later complications. Numerous medications are now available to treat low bone density. There is no complete agreement on the point at which treatment should be recommended.
Before every joint replacement surgery, a DEXA scan of the patient is required. The cost is low ($150). We have found that this test is very predictive of certain complications that can develop after surgery. Sometimes even very young patients can have low bone density. The result is used in hip resurfacing to determine the risk of postoperative femoral neck fracture and how to precisely prepare the socket in surgery. Patients who have weaker bones are treated with anti-resorptive medication and a longer period on crutches after the surgery. We have reduced the rate of complication of a femoral neck fracture from 1–2% to 0.1% using this strategy.
Metal Ion Level Testing for Hip Arthritis
Metal Ion Level testing is a valuable way to screen for excessive wear of metal-bearing implants. Every patient should have their cobalt, chromium, and titanium levels measured 2 years after surgery so that any problems with wear can be found early. In certain patients, we recommend repeat monitoring thereafter. Most patients who have metal-bearing hip replacements or metal-plastic-bearing knee replacements have elevated cobalt and chromium levels in their blood. There is no known problem caused by this.
Speculations of increased cancer risk have been disproven by numerous long-term studies. No evidence suggests that circulating ions can hurt the kidneys, but kidneys that don’t work right can cause the ion level in the blood to rise. There is no agreed-upon acceptable level for joint implant patients when we treat hip arthritis. The normal level in patients without implants is about 2 ug/L. We have done extensive studies on metal ion levels. We have seen an adverse wear failure (AWF) at 15 ug/L, which is the lowest level we have seen. Sometimes a level higher than this is seen without evidence for AWF.
Implant loosening may be another failure mode that can be associated with elevated levels. There have been a few reports of general systemic side effects that may have been caused by high levels of metal ions. We have seen more than 10 AWF cases with levels between 50 and 200 ug/L, and none exhibited any systemic symptoms. It appears that systemic effects do not occur at levels that are typically seen in well-functioning cases, and are even rare at the very high levels seen in AWF cases. We obtain levels at 2 years because it is known that implants go through a run-in wear period of 1-2 years. Less is known about what is an acceptable level during this time. The earliest time that we have ever seen an AWF is after 2 years; it takes time to develop these problems.
We currently recommend metal ion testing:
- Routinely on all patients at 2 years post-op
- When evaluating a painful hip implant
- Before performing a second hip surgery on the opposite hip
- Repeat levels periodically if levels are above 10 ug/L, there is a steep acetabular inclination angle, the patient has a recalled DePuy ASR implant
When we find an ion level above 10 ug/L, we tell people to get a metal suppression CT or MARS MRI. Significant soft tissue inflammatory masses (not cancer) or large fluid collections indicate a probable AWF. So far, AWF has only happened when the angle of tilt of the acetabulum is more than 50 degrees. However, only 5% of patients with AIA greater than 50 develop AWF.
Bone and Indium Scans
Bone and Indium scans are performed by removing some of your blood and labeling it with an isotropic material that is then re-injected. You will return one day later, and the area of the joint will be scanned. These tests assist us in determining implant loosening or infection. The amount of radiation is generally not much more than a single x-ray exposure. The complications have been minimal. Computerized scanning is sometimes combined with the injection of these agents to better define the changes in a three-dimensional way.
Aspiration & Arthrogram
Aspiration and Arthrogram are typically done to obtain information about the presence or absence of infection when we treat hip arthritis, particularly if you have had previous surgery. The radiologist might be able to take fluid from the hip joint directly, which would be very helpful. These samples can be analyzed by cell counts, culture gram stain, and PCR (a DNA test for bacteria).
Final culture results are usually available in 7–10 days. Most of the time, these procedures are not very painful because they use a local anesthetic on the skin. On occasion, mild discomfort may be associated with the study. Most often, it is transitory and can be relieved by medications.
Blood Tests
Blood tests such as CBC, CRP, and ESR are sometimes done as screening tests to rule out infection. If they are positive, we usually follow this up with either an indium scan and/or aspiration.